Pamiętacie film “Obcy. Ósmy pasażer Nostromo” , w którym istoty kosmiczne wgryzały się w organizmy członków załogi statku kosmicznego, a następnie powoli przejmowały kontrolę nad ich zachowaniem, pożerając przy tym od środka?
Jeśli myślicie Państwo, że taki scenariusz leży wyłącznie z sferze fantazji, popełniacie błąd. Obcy, pasażer na gapę jest blisko. Pełzające, zmiennokształtne istoty mogą wniknąć w nasze ciało, gdy jemy tatara lub krwisty stek. Obcy może nas zaatakować, gdy gdy kroimy mięso na tej samej desce, na której potem przygotowujemy inne jedzenie. Może przeniknąć do naszego organizmu przez odchody kota wychodzącego na dwór, bo to właśnie koty są głównym celem niewidzialnego wroga. Pasożyty, niewiele ustępujące zachowaniem ósmemu pasażerowi Nostromo, dostają się do przewodu pokarmowego zwierzęcia drogą pokarmową, czyli przez zakażone myszy i ptaki. Kotom toksoplazma krzywdy nie czyni, choć celem życiowym tego pasożyta jest dostanie się do kociego przewodu pokarmowego, gdzie może rozmnażać się płciowo, czyli wytwarzać gamety, zapładniać i w końcu wytwarzać oocysty, które wraz z brudem (np.: w przypadku nie umytych rąk) trafiają do ludzkich organizmów. Głaskanie futerka nie stwarza zagrożenia, jednak przypadkowy kontakt z kocimi odchodami niestety tak. Nie trzeba nawet mieć kota w domu i czyścić kuwety, bo zabrudzony może być np.: piasek w piaskownicy lub nawet warzywa.


Zarażenie i objawy u ludzi
Kot jest tak zwanym żywicielem ostatecznym. My, ludzie, podobnie jak wszystkie inne zwierzęta (w tym także te, które jadamy – krowy, barany, świnie, drób) jesteśmy żywicielami pośrednimi. Zakażony kot wydala oocyty zaledwie przez 3 tygodnie, jednak przetrwalniki mogą przeżyć nawet półtorej roku w wilgotnej glebie. Człowiek najczęściej zakaża się toksoplazmozą przez jedzenie mięsa. Objawy nie są charakterystyczne, przypominają grypę – lekka gorączka, bóle mięśni, rozbicie oraz czasem utrzymujące się powiększenie węzłów chłonnych.
W USA około 20% populacji może chorować na toksoplazmozę, tym bardziej, że niejednokrotnie zakażenie przebiega bezobjawowo. Jest to tym niebezpieczniejsze, że pod wpływem działania pasożytów w ludzkim organizmie może dojść do upośledzenia funkcjonowania układu odpornościowego, co prowadzi do tragicznych skutków.
Obcy przejmuje stery
Toksoplazmoza w takim przypadku zmienia sygnały w ośrodkowym układzie nerwowym, następnie prowadzi do zaburzeń funkcji mózgu, w tym napadów padaczkowych. Może ingerować w połączenia między neuronami.
Naukowcy z Bufallo odkryli, że pasożyt w tym celu posługuje się neuroprzekaźnikiem o nazwie kwas gamma-aminomasłowy, czyli GABA. Dzięki niemu może rozsiewać się w mózgu, w tzw. synapsach neuronów GABAergicznych, niszcząc je i zmieniając aktywność enzymu GAD67, od którego zależy produkcja GABA. Zaś wtórny niedobór kwasu gamma-aminomasłowego prowadzi do napadów padaczkowych.
Nie bój się! Masz zostać pożarty!
Badania wskazują, że Toxoplasma gondii ma wpływ na podejmowanie ryzyka i różne dziwne zachowania. Na przykład szczury zakażone toksoplazmozą nie boją się kotów – co oczywiście zmniejsza ich szanse na przeżycie. Pasożyt nie chce pozostać w przypadkowym ciele, dlatego steruje zachowaniem swego gospodarza pośredniego tak, aby zwiększyć ryzyko pożarcia przez żywiciela końcowego.
Brak strachu jest tylko jednym z czynników behawioralnych, powodowanych przez Toxoplasma gondii. Zmiany w neuroprzekaźnikach powodują również agresję, depresję i schizofrenię. Polski badacz prof. Prandota sugeruje, że autyzm dziecięcy może być skutkiem toksoplazmozy.
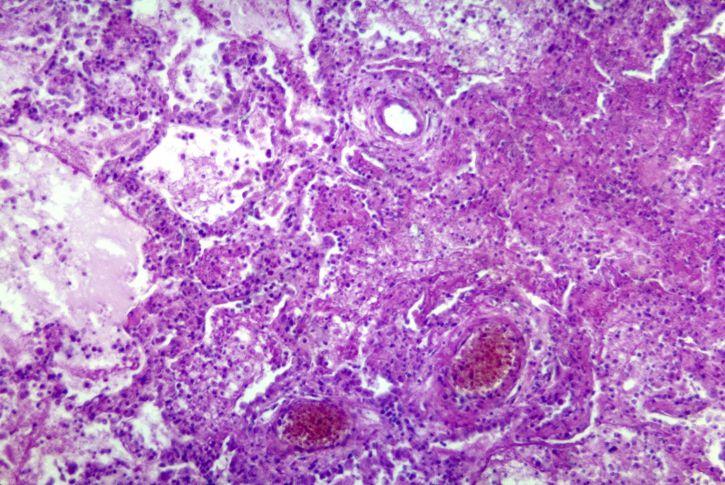

Zagrożenia
Do niedawna sądzono, iż toksoplazmoza jest zagrożeniem jedynie dla kobiet w ciąży, ponieważ powoduje wady płodu. Obecnie wiemy, że np.: postać oczna tego pasożyta może prowadzić do utraty wzroku. Postać mózgowa toksoplazmozy rozpoznawana jest rzadko, bo daje zmiany niecharakterystyczne. W medycynie pokutuje przekonanie, iż toksoplazmoza może być “przebyta”, czyli jeśli posiadamy przeciwciała IgG przeciwko temu pasożytowi, to wyleczyliśmy się z niego. Może być to prawdą jedynie u kotów.
Związek na zawsze
U ludzi pasożyt Toxoplasma gondii, jeśli wniknie raz do organizmu, pozostaje w nim na zawsze. W zależności od miejsca, w którym osiądzie, powoduje objawy lub pozostaje bezobjawowy. U osób ze sprawnym układem immunologicznym toksoplazmoza może zakończyć wędrówkę w węzłach chłonnych (postać węzłowa) oraz tworzy cysty, w których przetrwalniki czekają na okazję utraty odporności. U osób z osłabioną obroną organizmu wywołuje zakażenie oczu lub wielonarządowe. Śpiący w naszym ciele pasożyt może reaktywować się w sprzyjających warunkach i uaktywnić się na przykład podczas przeziębienia czy innej choroby.
Nie możemy zatem mówić więc o toksoplazmozie “przebytej i nieaktywnej”, musimy zawsze pamiętać, że gdy nastąpi zakażenie, pasożyt ten jest z nami na zawsze. Wiedzą o tym doskonale transplantolodzy, gdyż można ją przeszczepić np.: ze szpikiem.
Formy toksoplazmozy i drogi zakażenia
Żywiciel zaraża się drogą pokarmową. Obecne w oocyście pierwotniaki wydostają się w jelicie cienkim, następnie wnikają do komórek żernych (makrofagów) jelita swego żywiciela, gdzie mnożą się przez podział. Osobniki potomne, czyli tzw. tachyzoity mają zdolność ruchu – wędrują więc po organizmie, przenikają przez barierę jelitową do krwi i limfy, i tą drogą wnikają do komórek jądrzastych, w których intensywnie się rozmnażają. Stamtąd rozsiewają się do wielu narządów, takich jak centralny układ nerwowy, oko, mięśnie, serce i łożysko. To właśnie tachyzoity powodują reakcję immunologiczną organizmu gospodarza, dzięki czemu proces namnażania zostaje zahamowany. Zaatakowane przez układ odpornościowy tachyzoity przekształcają się w formy przetrwalnikowe, czyli bradyzoity. Skupiska bradyzoitów, tzw. cysty tkankowe występują w różnych miejscach, najczęściej w mózgu, oku i mięśniach. Bradyzoity są aktywne przez całe życie gospodarza. W momencie utraty odporności uwalniają się z cyst i ponownie przekształcają w formę inwazyjną – tachyzoity. Bradyzoity mnożą się bardzo wolno, toteż praktycznie nie poddają się leczeniu antybiotykowemu.
Bibliografia:
J. M. Fuks et al., GABAergic signaling is linked to a hypermigratory phenotype in dendritic cells infected by Toxoplasma gondii, PLoS Pathog., 8(12):e1003051, 2012 DOI: https://doi.org/ 10.1371/journal.ppat.1003051
G. Kannan and M. V. Pletnikov, Toxoplasma gondii and cognitive deficits in schizophrenia: An animal model perspective, Schizophr. Bull., 38(6):1155–1161, 2012 DOI: https://doi.org/ 10.1093/schbul/sbs079
G. A. McConkey et al., Toxoplasma gondii infection and behavior—location, location, location?, J. Exp. Biol., 216:113–119, 2013 DOI: https://doi.org/ 10.1242/jeb.074153
J. P. Webster et al., Toxoplasma gondii infection, from predation to schizophrenia: Can animal behaviour help us understand human behaviour?, J. Exp. Biol., 216:99–112, 2013 DOI: https://doi.org/ 10.1242/jeb.074716


WYSYŁKA BADAŃ
Najbliższe terminy wysyłek do Stanów (badania Metabolomix, Gi effects, CSA, CSAP2, Clostridium, Mikrobiologia, Uroporfiryny,
Badanie włosa, P. Cunningham, OAT)
kwiecień: 23.04.2024
maj: 14.05.2024, 28.05.2024
czerwiec: 11.06.2024, 25.06.2024
Próbki do badań wykonywanych w USA (mocz, kał, włosy, ślina) należy dostarczyć osobiście lub wysłać kurierem dzień wcześniej (zawsze są to poniedziałki), tak aby w terminie wysyłki dotarły do Arcany (zawsze we wtorki). Próbki do badań należy pobierać w weekend przed wysyłką, zgodnie z dołączonymi do zestawów instrukcjami.
Próbki surowicy do badań w CM Wielkoszyński można dostarczyć do Arcana w każdy poniedziałek (z wyjątkiem 01 oraz 29.04.2024) w godzinach otwarcia lub wtorek do godziny 15:00 z wyjątkiem tygodni, w które wypadają dni świąteczne lub instytut jest zamknięty.